
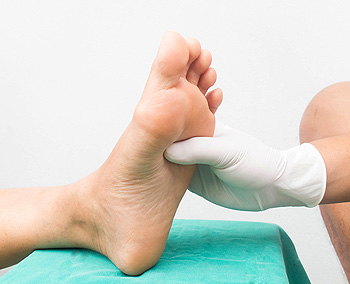
 Diabetes can often be accompanied by several serious foot ailments that can further threaten the health of those afflicted. For that reason, it’s a good idea for diabetic patients to develop a regular self-care regime to help protect their feet from developing ulcers, infections, and other painful conditions. First, it’s important to keep your feet clean and dry every day. Second, take time to inspect them for sores, cuts, bumps and bruises that might otherwise go unnoticed. Third, wear padded socks and shoes with non-slip soles. Also, keep your footwear clean and dry. Cracks in the skin, differences in foot temperature, pain, redness, swelling, tingling, or numbness may be signs of infections, nerve problems, or a decrease in blood flow. If you are experiencing any of these symptoms, it is a good idea to make visits to a podiatrist a regular part of your health care routine.
Diabetes can often be accompanied by several serious foot ailments that can further threaten the health of those afflicted. For that reason, it’s a good idea for diabetic patients to develop a regular self-care regime to help protect their feet from developing ulcers, infections, and other painful conditions. First, it’s important to keep your feet clean and dry every day. Second, take time to inspect them for sores, cuts, bumps and bruises that might otherwise go unnoticed. Third, wear padded socks and shoes with non-slip soles. Also, keep your footwear clean and dry. Cracks in the skin, differences in foot temperature, pain, redness, swelling, tingling, or numbness may be signs of infections, nerve problems, or a decrease in blood flow. If you are experiencing any of these symptoms, it is a good idea to make visits to a podiatrist a regular part of your health care routine.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Massimo Pietrantoni, DPM from Rochester Podiatry, LLP. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact one of our offices located in Brighton and Greece of Rochester, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetes can cause two problems that can potentially affect the feet: Diabetic neuropathy and Peripheral Vascular Disease. Diabetic neuropathy occurs when nerves in your legs and feet become damaged, which prevents you from feeling heat, cold, or pain. The problem with diabetic neuropathy is that a cut or sore on the foot may go unnoticed and the cut may eventually become infected. This condition is also a main cause of foot ulcers. Additionally, Peripheral vascular disease also affects blood flow in the body. Poor blood flow will cause sores and cuts to take longer to heal. Infections that don’t heal do to poor blood flow can potentially cause ulcers or gangrene.
There are certain foot problems that are more commonly found in people with diabetes such as Athlete’s foot, calluses, corns, blisters, bunions, foot ulcers, ingrown toenails, and plantar warts. These conditions can lead to infection and serious complications such as amputation. Fortunately, proper foot care can help prevent these foot problems before they progress into more serious complications.
Each day you should wash your feet in warm water with a mild soap. When you finish washing your feet, dry them carefully especially between your toes. You should also perform daily foot inspections to ensure you don’t have any redness, blisters, or calluses. Furthermore, if you are diabetic, you should always wear closed-toed shoes or slippers to protect your feet. Practicing these tips will help ensure that your feet are kept healthy and away from infection.
If you have diabetes, contact your podiatrist if you have any of the following symptoms on your feet: changes in skin color, corns or calluses, open sores that are slow to heal, unusual and persistent odor, or changes in skin temperature. Your podiatrist will do a thorough examination of your feet to help treat these problematic conditions.
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
Plantar fasciitis, an injury to the ligament that runs along the bottom of the foot, is one of the most frequently diagnosed conditions at the podiatrist’s office. In many cases, conservative treatments are offered to the patient and are typically sufficient for treating the injury. These may include resting and icing the affected foot, wearing more comfortable shoes or orthotics, doing gentle stretching exercises, and taking over-the-counter pain medications. While conservative treatments work for many patients, they aren’t completely effective for everyone. If you have heel pain that is severe enough to stop you from doing your daily activities, gets worse or keeps coming back, or has not improved after two weeks of conservative treatments, it is strongly suggested that you consult with a podiatrist. If you have diabetes, or any tingling or loss of sensation in the foot, it would be wise to seek the care of a podiatrist sooner, rather than later.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Massimo Pietrantoni, DPM from Rochester Podiatry, LLP. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact one of our offices located in Brighton and Greece of Rochester, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Corns are hard and thick areas of skin that form as a result of constant rubbing, friction, or pressure on the skin. They are patches of dead skin with a small plug toward the center. They may appear on the tops and sides of toes and can make walking painful.
Soft corns are typically thinner with a white color and rubbery texture. Soft corns tend to appear between the toes. Seed corns are another type of corn that appear in clusters and can be tender if they are on a weight-bearing part of the foot. Seed corns usually appear on the bottom of the foot and are likely caused by a blockage in sweat ducts.
While corns and calluses are somewhat similar, calluses are a bit different. Calluses are a patch of dead skin that can occur anywhere on the body. In comparison to corns, calluses are usually a bit larger in size. However, both corns and calluses are caused by increased friction on the skin.
There are some risk factors that may increase your chances of developing corns and calluses. If you have bunions, hammertoe, or a bone spur, you are more likely to develop a corn or callus on your foot.
While Corns and Calluses tend to disappear when the friction to the affected area ceases, the help of a podiatrist may be useful in the removal process. It is important to remove the dead skin around the area and this may be done in a few different ways. Moisturizing creams may be helpful in softening and removing the dead skin around the callus. You should never use razors or other pedicure equipment to remove your corns. Doing this may worsen your corn or callus and cause infection.
In some cases, corns and calluses may be caused by abnormal foot structure or walking motion. In such a case, you should seek a podiatrist’s assistance in order to correct the issue.
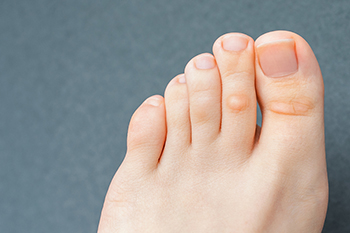 If you have pain on the top or side of your toe it may be caused by a hardened growth on the skin known as a corn, or heloma. Hard corns usually form if the toe repeatedly rubs against the side or top of your shoe. Soft corns can develop between the toes as they rub against each other when you walk. Sometimes these become infected. In both cases, the culprit is likely to be shoes that are too tight or pointy, causing the friction that forms into a corn. It’s not a good idea to cut or remove a corn yourself but soaking your feet in warm water to soften it may help. Then you can use a pumice stone, or nail file, to reduce the size of the corn. One of the main things you can do is to find shoes that help to reduce the friction. They should have a wider, roomy toe box and be made of a flexible material. If you frequently develop corns, it is a good idea to consult a podiatrist who can examine your feet, remove the corns, and offer treatment options to prevent them from recurring.
If you have pain on the top or side of your toe it may be caused by a hardened growth on the skin known as a corn, or heloma. Hard corns usually form if the toe repeatedly rubs against the side or top of your shoe. Soft corns can develop between the toes as they rub against each other when you walk. Sometimes these become infected. In both cases, the culprit is likely to be shoes that are too tight or pointy, causing the friction that forms into a corn. It’s not a good idea to cut or remove a corn yourself but soaking your feet in warm water to soften it may help. Then you can use a pumice stone, or nail file, to reduce the size of the corn. One of the main things you can do is to find shoes that help to reduce the friction. They should have a wider, roomy toe box and be made of a flexible material. If you frequently develop corns, it is a good idea to consult a podiatrist who can examine your feet, remove the corns, and offer treatment options to prevent them from recurring.
Corns can make walking very painful and should be treated immediately. If you have questions regarding your feet and ankles, contact Massimo Pietrantoni, DPM of Rochester Podiatry, LLP. Our doctor will treat your foot and ankle needs.
Corns: What Are They? And How Do You Get Rid of Them?
Corns are thickened areas on the skin that can become painful. They are caused by excessive pressure and friction on the skin. Corns press into the deeper layers of the skin and are usually round in shape.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as:
Treating Corns
Although most corns slowly disappear when the friction or pressure stops, this isn’t always the case. Consult with your podiatrist to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact one of our offices located in Brighton and Greece of Rochester, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Gout, typically found in diabetic patients, is an unusually painful form of arthritis caused by elevated levels of uric acid in the bloodstream. The condition typically strikes the big joint on the big toe. It has also been known to strike the knees, elbows, fingers, ankles and wrists—generally anywhere that has a functioning, moving joint.
The high level of uric acid in a person’s bloodstream creates the condition known as hyperuricema—the main cause of gout. Genetic predisposition occurs in nine out of ten sufferers. The children of parents who suffer gout will have a two in ten chance of developing the condition as well.
This form of arthritis, being particularly painful, is the leftover uric acid crystallizing in the blood stream. The crystallized uric acid then travels to the space between joints where they rub, causing friction when the patient moves. Symptoms include: pain, redness, swelling, and inflammation. Additional side effects may include fatigue and fever, although reports of these effects are very rare. Some patients have reported that pain may intensify when the temperature drops, such as when you sleep.
Most cases of gout are easily diagnosed by a podiatrist’s assessment of the various symptoms. Defined tests can also be performed. A blood test to detect elevated levels of uric acid is often used as well as an x-ray to diagnose visible and chronic gout.
Treatment for gout simply means eliminating symptoms. Non-steroid anti-inflammatory drugs or NSAIDs (Colchicine and other corticosteroid drugs, etc.) will quell the redness, the swelling, and the inflammation. However, managing your diet, lifestyle changes, and using preventative drugs are all helpful toward fully combating the most severe cases.
Those that lead an inactive lifestyle are at a higher risk for gout. Any amount of exercise decreases the probability of repeat encounters with the condition. Reducing your consumption of red meat, sea food, and fructose-sweetened drinks also reduces the likelihood of chronic gout as well.
Ingesting Vitamin C, coffee, and particular dairy products can help with maintaining a healthy lifestyle. There are new drugs out on the market that inhibit the body’s production of uric acid-producing enzymes. However, reducing or eliminating your overall levels of uric acid is the best remedy to ensuring you lead a gout-free life.
If you have ever suffered from a gout attack, a sudden and extremely painful inflammation of one or more joints in your foot, you may be surprised to find that one of the ways to manage symptoms and prevent future attacks is to modify your diet. Gout is caused by a buildup of a substance called uric acid in the bloodstream. This substance can crystallize and become lodged in a joint, leading to intense pain, swelling, and inflammation. Left untreated, repeated gout attacks can permanently damage the affected joints, causing chronic pain and restricting their range of motion. Purines are chemical compounds naturally found in certain foods. In the body, purines get converted to uric acid. When there are too many purines, they can create excess uric acid that builds up in the body, increasing your risk of having a gout attack. By avoiding foods and drinks with large amounts of purine, you may be able to lower your risk of gout. Foods to avoid include red and organ meats, certain types of seafood, highly processed or sugary foods, and yeast. You should also avoid drinking sugary or alcoholic beverages. For more information about the relationship between your diet and your foot health, please consult with a podiatrist.
Gout is a foot condition that requires certain treatment and care. If you are seeking treatment, contact Massimo Pietrantoni, DPM from Rochester Podiatry, LLP. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a type of arthritis caused by a buildup of uric acid in the bloodstream. It often develops in the foot, especially the big toe area, although it can manifest in other parts of the body as well. Gout can make walking and standing very painful and is especially common in diabetics and the obese.
People typically get gout because of a poor diet. Genetic predisposition is also a factor. The children of parents who have had gout frequently have a chance of developing it themselves.
Gout can easily be identified by redness and inflammation of the big toe and the surrounding areas of the foot. Other symptoms include extreme fatigue, joint pain, and running high fevers. Sometimes corticosteroid drugs can be prescribed to treat gout, but the best way to combat this disease is to get more exercise and eat a better diet.
If you have any questions please feel free to contact one of our offices located in Brighton and Greece of Rochester, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.